
Ever experienced a stomach ache during a stressful time? Or joint pain when feeling down? That’s somatization – where emotional distress takes a physical form. From everyday headaches to impairments in physical functioning, somatization can vary for each individual. It can be a temporary response to stress or a more prolonged experience affecting your overall well-being. Understanding this spectrum helps us navigate the mind-body connection.
The Mind-Body Connection: How Emotions Manifest in the Body
Somatization refers to the phenomenon of psychological or emotional distress manifesting as physical symptoms (“Somatization”, GoodTherapy). For example, high anxiety might manifest as a stomach ache or nausea, grief might manifest as severe fatigue, and depression might manifest as joint pain. The symptoms will vary in duration, frequency, and intensity, as well as between individuals. In most cases, somatization will be temporary and situational. While an organic cause may not be found to explain physical symptoms, somatization and the subsequent distress are valid experiences. Similar to many psychological conditions, somatization is understood as a spectrum (Servan-Schreiber, Kolb, and Tabas, 2000). At the low end, physical symptoms such as headaches and lower back pain may emerge during a stressful situation such as a divorce or new job. At the high end, physical symptoms can leave people with impairments in physical, social, and occupational functioning.
Theories on What Causes Somatic Symptoms:
- Some people have higher sensitivity to physical sensations such as pain or nausea.
Strong psychological distress can stimulate receptors to mimic the sensation of pain. - Hormones such as cortisol are released during stressful and traumatic situations. The immune system might weaken during stress and evoke physical symptoms.
- Somatization can be interpreted as a defense mechanism against emotional overwhelm. Lacking appropriate support and outlet, emotional and psychological conflicts convert into physical symptoms. Then, the physical symptoms draw attention and can be treated while the mind detaches from the psychic conflicts.
- The role of stigma or cultural expectations can act as a barrier to displaying emotional and psychological symptoms. Often, physical symptoms receive preferential treatment and attention over psychological pain. Hence, emotional and psychological problems might become visible via physical symptoms in the body in order to locate healing.
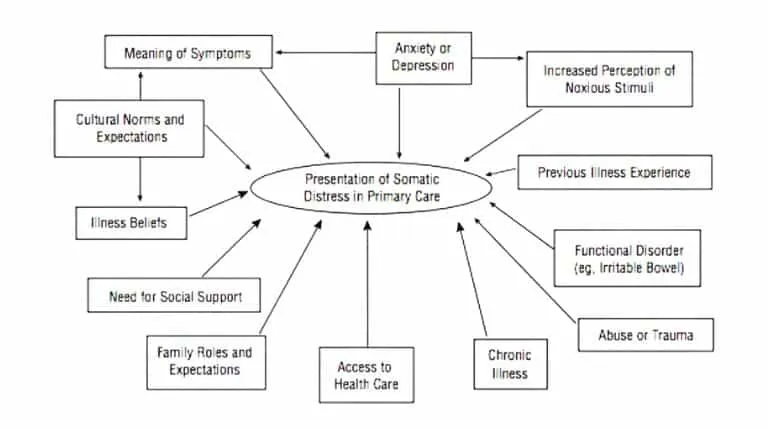
Biopsychosocial model of somatic stress, diagram from Epstein, Quill, and McWhinney (1999)
Examples of Somatic Symptoms caused by Stress:
Musculoskeletal system
Common somatization reported: hurting overall, pain in extremities, back/joint pain, pain during urination, headaches (Blackwell and DeMorgan, 1996); Stress is stored throughout the human body. While one can handle small doses of stress, significant and long-term stress can leave a toxic effect on the body. Muscles become tense during times of stress and can remain tense following prolonged exposure to stress. Long-term muscle tension around the head, neck, and shoulders, for instance, are associated with tension-type headaches and migraines. Similarly, lower back pain and pain in the upper extremities are associated with stress, specifically stress related to employment.
Respiratory system
Common somatization reported: dizziness, chest pain, shortness of breath at rest (Blackwell and DeMorgan, 1996); During times of high stress or anxiety, the body enters fight or flight mode and normal breathing patterns become disrupted (e.g. shortness of breath, hyperventilation). Hyperventilation or rapid breathing occurred because this process oxygenates blood and prepares the body to fight or flee whatever threat they’re facing. Sometimes thoughts and emotions can be so stressful and anxiety-provoking that they trigger a physical response as if the threat were real and dangerous. On the other hand, rapid heart palpitations caused by stress and anxiety can induce shortness of breath or even dizziness.
Cardiovascular system
Common somatization reported: palpitations (Blackwell and DeMorgan, 1996); Stress can increase heart rate and contractions of the heart muscles, provoking the release of stress hormones such as adrenaline and cortisol. Blood pressure also increases due to dilation of blood vessels, causing increased blood to the heart. The body should return to homeostasis when stress subsides; however chronic stress extends the overactivity of the heart and vessels, increasing the chance of hypertension, stroke, or even heart attack. Chronic and persistent stress yields to inflammation of coronary arteries which yields to a heart attack.
Endocrine system
Stressful situations activate the hypothalamus-pituitary-adrenal (HPA) axis, a cascade of events increasing production and release of steroid hormones such as cortisol. Cortisol is referred to as a “stress hormone” and acts as fuel for adaptation to stress. The “stress hormone” helps lower inflammation while regulating the immune system since stressful situations may induce a spike in immune system activation. Prolonged stress has the potential to disrupt the link between the immune system and HPA axis, leading to a number of problems such as fatigue, diabetes, obesity, depression, anxiety, and immune disorders.
Gastrointestinal system
Common somatization reported: vomiting, abdominal pain, nausea, bloating and excessive gas, diarrhea, food intolerance (Blackwell and DeMorgan, 1996). Our gut and microbiome communicate with the brain. The gut and brain are influenced by stress, such that they may contribute to pain sensation, bloating, and other gut-related irregularities. Additionally, the microbiome can influence cognition and affect. Stress is known to induce mood-altering changes in gut microbiome.
Nervous system
Common somatization reported: pseudoneurological symptoms such as amnesia, difficulty swallowing, loss of voice, deafness, double or blurred vision, blindness, fainting, difficulty walking, seizures, muscle weakness, difficulty urinating (Blackwell and DeMorgan, 1996); Long-term stress perpetuates continuous physical reactions in the autonomic nervous system, increasing the wear-and-tear on the body and bodily systems.
Reproductive system
Common somatization reported: burning sensations in sexual organs, dyspareunia, painful menstruation, irregular menstrual cycles, excessive menstrual bleeding, vomiting throughout pregnancy (Blackwell and DeMorgan, 1996);
- For males: chronic stress influences testosterone production, which can decrease sex drive, produce erectile dysfunction or impotence. Additionally, stress can decrease sperm production and maturation, with impact affecting the motility and morphology of sperm. Lastly, stress can compromise the immune system, making the body vulnerable to infection and disease.
- For females: stress can affect menstruation and reduce sexual desire. Chronic stress can increase the chance of depression and anxiety developing during pregnancy and postpartum adjustment. Stress can exacerbate the course of reproductive diseases
Syndromes reported for somatization: vague “food allergies”, atypical chest pain, jaw muscle pain, “hypoglycemia”, chronic fatigue syndrome, fibromyalgia, vague “vitamin deficiency”, premenstrual syndrome, multiple chemical sensitivity (Blackwell and DeMorgan, 1996).
(“Stress Effects on the Body”, APA)
How to Cope with Chronic Stress and Avoid Somatic Symptoms:
1. Develop a relaxation routine
- Deep abdominal breathing, visualization of a peaceful place, prayer, yoga, tai chi
2. Engage in physical activity
- Walking, running, yoga, tai chi, qi gong
3. Develop social support
- Friends, confidants, coworkers, partners, family members, neighbors, etc
(“Understanding the Stress Response.” Harvard)
References
1. Blackwell, B., & DeMorgan, N. (1996). The primary care of patients who have bodily concerns. Archives of Family Medicine, 5(8), 457–463. https://doi.org/10.1001/archfami.5.8.457
2. Epstein, R.M., Quill, T.E., McWhinney, I.R. (1999). Somatization reconsidered. Archives of Internal Medicine, 159, 215–222.
3. Servan-Schreiber, D., & Kolb, N.R, Tabas, G. (2000). Somatizing patients: Part 1 practical diagnosis. American Family Physician, 61(4), 1073–1078.
4. “Somatization.” GoodTherapy, GoodTherapy LLC, 26 July 2019, http://tinyurl.com/nrr2d32a
5. “Stress Effects on the Body.” American Psychological Association, American Psychological Association, 8 Mar. 2023,. www.apa.org/topics/stress/body
6. “Understanding the Stress Response.” Harvard Medical School, Harvard Health, 6 July 2020,. www.health.harvard.edu/staying-healthy/understanding-the-stress-response











